Urticaria is the medical term for hives, which can appear as a raised itchy rash on the skin.
Urticaria is the medical term for hives, which can appear as a raised itchy rash on the skin.
Urticaria is the medical term for hives, which can appear as a raised itchy rash on the skin; this page initially discusses four types of urticaria:
Lower down, this page will go on to focus on urticaria that is both chronic and spontaneous, also known as chronic spontaneous urticaria or CSU.
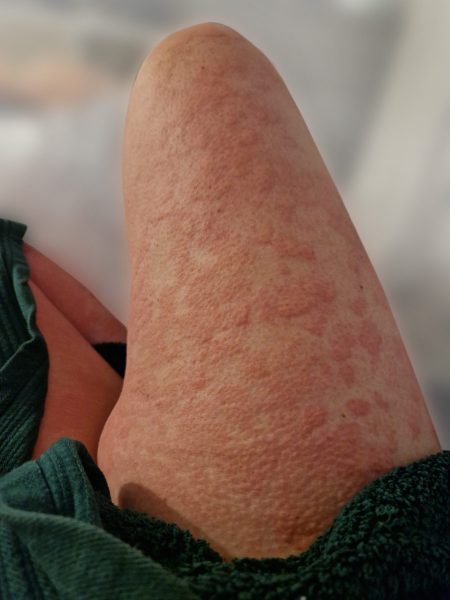
Most people will have an outbreak of hives at some point in their lives. In the majority of cases, this is short-lived and hives are completely gone within a few days. This type of urticaria is known as acute urticaria. When people have hives that come and go for longer than 6 weeks, it is called chronic urticaria.
There are different types of chronic urticaria including spontaneous urticaria and physical urticaria.
Spontaneous urticaria does not have a clear trigger. It is not caused by foods or medicines and symptoms can occur ‘out of the blue’, without a clear cause.
Physical urticaria (sometimes called inducible urticaria) is where hives occur when exposed to a specific physical trigger, for example a change in temperature or pressure. One type of physical urticaria is ‘cold urticaria’. People with cold urticaria might find that their symptoms are triggered by very cold weather or by jumping into cold water. Another type of physical urticaria is pressure-induced urticaria. You might find that you get hives where your clothing is tight, e.g. underneath bra straps or at the waist of tight fitting trousers.
Lots of people with urticaria will find that they experience both spontaneous urticaria and physical urticaria. No matter what kind of urticaria you have, the initial treatments are largely the same. You can discuss your specific type of urticaria with your doctor.
CSU refers to hives that come and go, without any particular or obvious trigger, and last for longer than 6 weeks.
For people with CSU, skin rashes can come and go over long periods of time. The urticaria (hives) are described as ‘spontaneous’ because of their unpredictability and the fact that they are not caused by food or medicines.
Cells in our body called mast cells are important in the development of hives and swellings. Mast cells are present all over the body and some are in our skin. These cells contain high amounts of naturally occurring histamine. When mast cells release their histamine, the blood vessels around them widen and increase blood flow to the area. The release of histamine is what causes itchy hives.
Increased blood flow to the skin surrounding hives can cause redness. The blood vessels involved can leak fluid and this can make a hive or wheal appear ‘raised’. In some cases, the same process happens in the deeper layers of the skin and this causes swellings (angioedema). Angioedema is the medical term for soft tissue swelling.
Mast cells in our skin can be affected by things like stress or naturally occurring hormones in our body. This is why people may experience a flare in their urticaria at times of stress or hormonal fluctuation. You may find that there are factors that can make your urticaria worse. These are different for everyone but can include an infection (e.g. a cough or a cold), the menstrual cycle, alcohol consumption, exercise or heat. Although food and medicines do not cause CSU, anti-inflammatory medications such as ibuprofen, can also be a trigger for some people with CSU.
Certain types of urticaria can also be triggered by autoimmunity, where substances that occur naturally in our body can make mast cells more active than they should be.
The swellings associated with CSU, known as angioedema, typically affect the eyes or lips but can affect any part of the body. These swellings can understandably be very distressing and distracting for patients. They can also naturally cause worry for patients if they occur in areas such as your tongue or throat. The treatment for hives and swellings is the same. Once you start appropriate treatment, your symptoms should start to improve.
CSU is common, affecting about 1 in 100 people. It is four times more common in females. Most people with CSU are otherwise healthy.
If you feel you have symptoms of chronic spontaneous urticaria, you should discuss this with your GP. As part of the accurate diagnosis of urticaria, your GP will take a detailed history and perform a physical examination. Your GP will likely ask you about any regular medicines you are taking and also any over the counter medicines. It is a good idea to take pictures of your rash and swellings, to show to your doctor. Your GP may refer you to a specialist if it is deemed appropriate.
The ISF have developed step-by-step guides; one for Family doctor/GP visits and a second for Hospital visits about your psoriasis. These can help you to prepare for your next appointment.

No. CSU is not an allergy to food or medications. One of the difficulties of living with hives and swellings is that these symptoms can frequently be confused with an allergic reaction. This is understandable as the appearance of hives and swellings are similar to those seen in an allergic reaction. However, allergic reactions happen very soon after the food or medicine that caused them, typically within minutes and always within 2 hours. Spontaneous hives and swellings, on the other hand, can come and go at any time.
People who get hives or swellings can understandably get frustrated looking for a cause or an ‘answer’ to what is causing their symptoms. CSU, however, like lots of conditions, is a skin disease where there is no one ‘answer’. Instead there are lots of contributing factors. Doctors and scientists are trying to understand the disease better to improve treatments.
IgE is a type of immune cell that can be higher in people with allergic diseases, for example hay fever. Some people with CSU will have an elevated IgE on blood testing. This is not a particular cause for concern. Food allergy testing can involve a blood test for a specific IgE which acts as a radar for a particular allergen.
As CSU is not caused by food allergens, allergy testing (IgE sensitisation testing or skin prick testing) is generally not needed. A doctor with experience in allergic conditions will be able to talk to you about your symptoms to determine what further steps you need to take.
Hives and swellings can be alarming and upsetting. This is particularly the case if swellings affect the mouth or throat. However, the swellings that occur as part of CSU are quite different to the swellings seen in allergic reactions. Life-threatening swellings of the throat are extremely unlikely in people with CSU.
An EpiPen (adrenaline autoinjector) is not a routine part of treatment for individuals with CSU. Your doctor will discuss this with you and can provide plans on how to manage all symptoms effectively.
Hives and swellings are normally managed with antihistamine tablets. These are typically used at higher doses than in other conditions. There are lots of different types of anti-histamines. CSU is commonly treated with long acting, non-sedating anti-histamines. In some cases, different anti-histamines are used in combination to help control your symptoms.
Biologic drugs that target IgE are used in hives and swellings that do not respond to standard treatment. Anti IgE treatments are typically given as an injection that you take once a month. These medicines are currently only available to patients who are under specialist services in certain hospitals.
In a small number of cases, drugs that suppress the immune system, like ciclosporin are used.
After taking a history of your condition, your doctor can help develop a management plan with you that meets your needs.
Not at this point in time. The treatments used for CSU should manage your symptoms effectively. You should know that hives and swellings may disappear on their own. 50% of people with spontaneous hives and swellings will stop having flares within a year.
If your hives and swellings do not go away on their own, that does not necessarily mean your symptoms will get worse over time. For people whose hives and swellings are ongoing, finding the right treatment that fits your needs is important.

Some people with CSU find that emotional stress can make their rash and swellings worse. This is not surprising as stress can have a negative impact on lots of medical conditions.
Outside of this, you may also find that your urticaria causes you stress. You may find the appearance of hives and swellings difficult to manage. There can be embarrassment about how symptoms look to other people.
Trying to pinpoint a cause or a trigger can be exhausting. These feelings in turn can cause distress which reduces our ability to cope and problem solve effectively. The cycle of stress therefore is important to acknowledge when we think about managing hives and swellings.
Improving psychological wellbeing is an important part of treating hives and swellings.
In Ireland, new techniques such as mindfulness and attention-based training are being used to try and reduce symptoms of itch and swellings. These techniques can help us to focus on what is happening in the present moment and to be compassionate with ourselves. These approaches will hopefully become part of routine care for patients with urticaria and angioedema.
You can ask your doctor for help with these issues if you think stress is a trigger for your hives and swellings. The importance of stress as a factor which contributes to urticaria should not be underestimated.

Sometimes, it’s not possible to find a cause of CSU, but in some people with CSU, they can have their symptoms provoked or aggravated by certain triggers. Some triggers may include; certain medications, heat, cold, pressure, physical and emotional stress. Triggers differ between individuals.
Other reliable sources of patient information include: